Informed academics and medical practitioners are unanimous that a clean-up of the malodorous augean stables of the medical profession must begin with comprehensive disinfestation of the Medical Council of India, from which the contagion has filtered into the bloodstream of medical education and practice. Summiya Yasmeen & Swati Roy report
 Medical education in the country is in coma. A rash of scams in the nation’s 355 medical colleges and the apex-level Medical Council of India (MCI, estb. 1934), has cast an ominous shadow over the medical profession, its dubious prac-tices, ethics and commitment to the Hippocratic oath.
Medical education in the country is in coma. A rash of scams in the nation’s 355 medical colleges and the apex-level Medical Council of India (MCI, estb. 1934), has cast an ominous shadow over the medical profession, its dubious prac-tices, ethics and commitment to the Hippocratic oath.
On July 17, the Central Bureau of Investigation (CBI) filed chargesheets against six medical colleges which received approval from MCI to increase capacity and introduce postgraduate programmes, despite being patently unqualified in terms of infrastructure and faculty. MCI’s reckless licensing of new colleges, permitting arbitrary increases of student admissions and approval of postgraduate programmes in medical colleges during the past decade, has raised serious doubts about the quality and competence of the country’s 816,629 practitioners of allopathic medicine who tend to dismiss India’s estimated 752,254 practitioners of alternative medicine (ayurvedic, unani, etc) as quacks.
The recent flood of scandals in medical education and horror stories about medicine as practised in govern-ment hospitals graphically depicted on television screens across the country, has prompted even the usually taciturn prime minister Dr. Manmohan Singh to speak up. “There’s a perception of deteriorating quality. We cannot allow this situation to continue. We must put in place a credible regulatory and institutional mechanism to help develop standards in our medical education,” he said, while addressing students at the third convocation of the Jawaharlal Institute of Post Graduate Medical Education and Research (JIPMER), Puducherry on June 29.
Conceding that contemporary India has perhaps the worst doctor-population ratio (1:1,700) worldwide, Singh announced a major capacity expansion drive in medical education. Six AIIMS (All India Institute of Medical Sciences)-like institutions will become operational in Bhopal, Bhubaneswar, Jodhpur, Patna, Raipur and Rishikesh in 2012-2013 offering 50 MBBS seats each, and the country’s 355 medical colleges — which qualify a mere 41,469 MBBS graduates annually — will be permitted to promote branch campuses in under-served states such as Bihar, Jharkhand, Chhattisgarh, West Bengal, Rajasthan, Uttar Pradesh, Madhya Pradesh and in north-east India. Moreover during the past two years, the Union ministry of health and family welfare, which reconstituted MCI with its nominees, has sanctioned 2,400 MBBS seats in 20 new medical colleges and 1,195 additional seats in existing colleges countrywide.
 However this capacity expansion drive has failed to enthuse the medical fraternity or public. With police and CBI investigations continuously exposing the medical colleges-MCI corruption nexus, there’s apprehension about the competence and professional capability of the 41,469 MBBS graduates churned out annually. “In the current scenario when there are big question marks over the authenticity and validity of MCI’s approval and licensing processes, inaugurating new medical colleges and increasing student intake could result in further deterioration of quality of MBBS and postgrad medical practiti-oners. Several sub-standard colleges with suspect credentials have received MCI approval to increase student intake and introduce postgraduate progra-mmes, whereas reputable medical colleges have been denied permission. Pervasive corruption, a severe shortage of quality faculty, and obsolete curri-culums have tarnished the quality of education dispensed by India’s medical colleges. The clean-up must begin with MCI which has to quickly rebuild its reputation and establish transparent licensing and recognition processes and systems,” says Dr. Mukesh Yadav, professor and head of department of forensic medicine and toxicology at Sharda University, Greater Noida (Uttar Pradesh) and founder-convenor of Quality of Medical Education, an online Yahoo group with a membership of 7,500.
However this capacity expansion drive has failed to enthuse the medical fraternity or public. With police and CBI investigations continuously exposing the medical colleges-MCI corruption nexus, there’s apprehension about the competence and professional capability of the 41,469 MBBS graduates churned out annually. “In the current scenario when there are big question marks over the authenticity and validity of MCI’s approval and licensing processes, inaugurating new medical colleges and increasing student intake could result in further deterioration of quality of MBBS and postgrad medical practiti-oners. Several sub-standard colleges with suspect credentials have received MCI approval to increase student intake and introduce postgraduate progra-mmes, whereas reputable medical colleges have been denied permission. Pervasive corruption, a severe shortage of quality faculty, and obsolete curri-culums have tarnished the quality of education dispensed by India’s medical colleges. The clean-up must begin with MCI which has to quickly rebuild its reputation and establish transparent licensing and recognition processes and systems,” says Dr. Mukesh Yadav, professor and head of department of forensic medicine and toxicology at Sharda University, Greater Noida (Uttar Pradesh) and founder-convenor of Quality of Medical Education, an online Yahoo group with a membership of 7,500.
Informed academics and conscien-tious medical practitioners are unani-mous that a clean-up of the malodorous augean stables of the medical prof-ession must begin with comprehensive disinfestation of the Medical Council of India, from which the contagion has filtered into the bloodstream of medical education and practice.
Established in pre-independence India under the Indian Medical Council (IMC) Act, 1933, MCI’s initial brief was to prescribe uniform standards for allopathic medical educ-ation and licence medical practitioners. The IMC Act of 1933 was repealed in 1956 and replaced with the Indian Medical Council Act (amended in 1964, 1993, 2001 and 2011) which expanded MCI’s powers, investing it with the authority to recognise/de-recognise medical colleges and their degrees; stipulate academic and faculty stand-ards; inspect colleges to evaluate infrastructure adequacy; approve new study programmes and authorise additional student intake. With private entrepreneurs entering professional education in a big way to promote medical and engineering colleges in the 1980s, MCI began to slide into corruption, cronyism and licence-permit-quota raj.
Matters came to a head during the tenure of Ketan Desai, an obscure professor of urology at B.J. Medical College, Ahmedabad, who was elected MCI president in 1996. During his five-year tenure (1996-2001), Desai allegedly amassed a huge fortune including a Rs.10 crore bungalow in Ahm-edabad by brazenly auctioning MCI’s licensing, recognition and discretionary powers. On November 23, 2001 in Union of India vs. Dr. Harish Bhalla & Ors and Dr. Ketan Desai vs. Dr. Harish Bhalla & Ors, the Delhi high court convicted Desai for accepting a bribe of Rs.65 lakh from two businessmen in Delhi for dispensing favours to two medical colleges in Pimpri and Ghaziabad, and ordered his removal from the presidency of MCI. The court directed the CBI to probe and prosecute Desai under the Prevention of Corruption Act, 1988.
 In its judgement, the Delhi high court bench comprising justices A. Kumar and R. Chopra also sternly reprimanded the Central government, which it held responsible for the composition of MCI and its failure to ensure a balance between elected and nominated members. “It is obvious from the record that the Central government has not at all made bona fide efforts or adopted effective measures to ensure that the quota of elected members in the MCI is filled. The council has a majority of nominated members owing allegiance to those who nominate them. The fact that respondent No.3 (Desai) won the election as president with such an overwhelming majority proves that the control of the council is being manoeuvred by such tactics… Desai enjoys a special clout with concerned government officials,” observed the court.
In its judgement, the Delhi high court bench comprising justices A. Kumar and R. Chopra also sternly reprimanded the Central government, which it held responsible for the composition of MCI and its failure to ensure a balance between elected and nominated members. “It is obvious from the record that the Central government has not at all made bona fide efforts or adopted effective measures to ensure that the quota of elected members in the MCI is filled. The council has a majority of nominated members owing allegiance to those who nominate them. The fact that respondent No.3 (Desai) won the election as president with such an overwhelming majority proves that the control of the council is being manoeuvred by such tactics… Desai enjoys a special clout with concerned government officials,” observed the court.
Desai’s “special clout with concerned (sic) government officials” ensured that the CBI didn’t make headway in its investigations. In 2005, CBI filed a closure report in the case stating that the Rs.65 lakh taken by Desai was “goodwill” money. Four years later in 2009, an emboldened Desai, who through his cronies had held a vice-like grip over MCI despite his ouster in 2001, was re-elected MCI president. But a reported fall-out with his protectors (i.e. politicians and bureaucrats) in the Central government resulted in his being arrested again a year later and charged with corruption. On April 22, 2010, the CBI arrested Desai for accepting a bribe of Rs.2 crore for granting MCI recognition to a private medical college in Patiala.
 In this context of high-level politicking and corruption, it’s pertinent to note that during Desai’s infamous 14-year reign which ended in 2010, MCI licensed and ‘recognised’ 35 new medical colleges, most of them with grossly inadequate infrastructure and faculty, while some of the country’s most respected medical colleges — including the pioneer Kasturba Medical College, Manipal (estb. 1953) — were briefly derecognised. Licence-permit-quota raj was used to infuse fear in private college managements which didn’t pay protection money. Simultaneously, capacity in colleges countrywide was capped to widen the demand-suppy gap and push illegal capitation fees higher.
In this context of high-level politicking and corruption, it’s pertinent to note that during Desai’s infamous 14-year reign which ended in 2010, MCI licensed and ‘recognised’ 35 new medical colleges, most of them with grossly inadequate infrastructure and faculty, while some of the country’s most respected medical colleges — including the pioneer Kasturba Medical College, Manipal (estb. 1953) — were briefly derecognised. Licence-permit-quota raj was used to infuse fear in private college managements which didn’t pay protection money. Simultaneously, capacity in colleges countrywide was capped to widen the demand-suppy gap and push illegal capitation fees higher.
“You can’t do without Dr. Desai if you run a private medical college in the country. You either have him or his nominee on the board of management if you want to circumvent merit and sell an estimated 2,500 coun-trywide ‘management quota’ seats available in MBBS colleges, despite an explicit Supreme Court ban on capitation fee. At a conser-vative average of Rs.20 lakh per seat, the management quotas fetch capitation fees worth a staggering Rs.500 crore annually and the busi-ness has steadily grown during the years Desai has been in power,” wrote a Times of India reporter (TOI, June 8, 2009).
Following a national furore after Desai’s shenanigans became public knowledge, the Medical Council of India was dissolved by an ordinance signed by President Pratibha Patil on May 13, 2010, and the Central government was authorised to constitute a six-member Board of Governors (BoG) with a one-year term. Subsequently the Union health ministry constituted a new board under the chairmanship of eminent gastroenterologist Dr. S.K. Sarin.
The BoG’s tenure expired in May last year and a newfour member board was reconstituted under the chair-manship of Dr. K.K. Talwar, former director of the Post Graduate Institute of Medical Research, Chandigarh. Despite allegations of corruption within MCI under the present BoG headed by Dr. Talwar, Union health minister Dr. Ghulam Nabi Azad has extended its tenure by another year. On July 17, the CBI filed chargesheets against six medical colleges which received approval from MCI’s current BoG to increase their intake and intro-duce postgraduate courses “despite flouting norms”. Dr. Talwar failed to respond to several telephone calls and e-mails sent by your correspondents.
 “The problems of MCI are many. Its reconstitution is irrelevant and inconsequential. The entire regulatory and licensing process needs to be overhauled with the government and council playing a facilitative role. Currently, 27 approvals are required to promote a new private medical college and any existing medical college which wants to introduce a new postgraduate programme or increase student intake is obliged to obtain prior MCI approval. The many conditions, some of which are completely unnecessary for establishing new medical colleges or expanding capacity, must be rationalised to create a transparent approval proc-ess. For instance, capacity expansion in medical education would receive a big boost if sharing of hospital facilities and resources is allowed between medical colleges located within a specified radius. Moreover, MCI needs to urgently reform the MBBS syllabus to make it contem-porary, and integrate clinical skills, ethics and soft skills education into it. The national outrage over MCI is a good opportunity to overhaul the medical education system in this country. But for this to happen, politicians must let go of control and leave the management of MCI to academicians,” says Dr. S. Kumar, president (medical education) of the Gokula Education Foundation which runs the top-rung M.S. Ramaiah Medical College, Bangalore (estb.1979) with an enrolment of 1,000-plus und-ergraduate and postgraduate students.
“The problems of MCI are many. Its reconstitution is irrelevant and inconsequential. The entire regulatory and licensing process needs to be overhauled with the government and council playing a facilitative role. Currently, 27 approvals are required to promote a new private medical college and any existing medical college which wants to introduce a new postgraduate programme or increase student intake is obliged to obtain prior MCI approval. The many conditions, some of which are completely unnecessary for establishing new medical colleges or expanding capacity, must be rationalised to create a transparent approval proc-ess. For instance, capacity expansion in medical education would receive a big boost if sharing of hospital facilities and resources is allowed between medical colleges located within a specified radius. Moreover, MCI needs to urgently reform the MBBS syllabus to make it contem-porary, and integrate clinical skills, ethics and soft skills education into it. The national outrage over MCI is a good opportunity to overhaul the medical education system in this country. But for this to happen, politicians must let go of control and leave the management of MCI to academicians,” says Dr. S. Kumar, president (medical education) of the Gokula Education Foundation which runs the top-rung M.S. Ramaiah Medical College, Bangalore (estb.1979) with an enrolment of 1,000-plus und-ergraduate and postgraduate students.
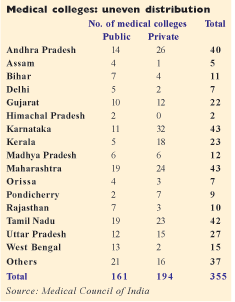
According to Kumar, the four southern states (Karn-ataka, Tamil Nadu, Kerala and Andhra Pradesh) and the western state of Maharashtra, together host 80 percent of the medical colleges in the country, while the rest of India is starved of them. For instance Uttar Pradesh — India’s most populous state (200 million) — has a mere 27 medical colleges; Madhya Pradesh (pop. 72 million) 12 and West Bengal (pop. 90 million) 15 (see box). According to the World Health Organisation, the doctor-population ratio in India is 1:1,700 (cf. the world ratio of 1.5:1,000). “Poor planning by government is responsible for this grossly uneven geographical distribution of medical colleges. It has created a severe demand-supply imbalance in medical education in the under-served states of north, central and eastern India,” says Kumar.
The West Bengal state government led by Mamata Banerjee of the Trinamool Congress, which ended 34 years of uninterrupted rule of the Communist Party of India-Marxist (CPI-M) led Left Front government in the assembly elections of May 2011, recently announced five new medical colleges in the public-private partnership (PPP) mode in the state. “It’s impossible to deny that the number of medical colleges in the state is highly inadequate. Of the 15 medical colleges in the state, only two are in the private sector. The Trinamool Congress government has decided to promote five more medical colleges in the PPP mode with immediate effect. This will to some extent remedy the situation, but plans to promote more medical colleges need to be drawn up right now,” says Prof. (Dr.) L.K. Ghosh, dean of modern medicine at the West Bengal University of Health Sciences.
 However, it’s pertinent to note that students enroled in West Bengal’s 13 government medical colleges pay a tuition fee of a mere Rs.750 per month (i.e Rs.9,000 per year). Abysmally low tuition fees in govern-ment medical colleges which require massive subsidies from state govern-ments with large fiscal and budgetary deficits is not peculiar to West Bengal; it’s a countrywide phenomenon. In the premier government-run AIIMS, Delhi, the tuition fee is Rs.1,350 per year (A 2009 study Determination of the cost of training of MBBS student at AIIMS conducted by its department of hospital administration, estimates the cost of education provision in this top institute at Rs.31.31 lakh per annum per student). In Maharashtra, the government-run Seth Gordhandas Sunderdas Medical College in Mumbai, which has an enrolment of 2,000 undergraduate and postgrad students, charges tuition fees of Rs.20,000 per year.
However, it’s pertinent to note that students enroled in West Bengal’s 13 government medical colleges pay a tuition fee of a mere Rs.750 per month (i.e Rs.9,000 per year). Abysmally low tuition fees in govern-ment medical colleges which require massive subsidies from state govern-ments with large fiscal and budgetary deficits is not peculiar to West Bengal; it’s a countrywide phenomenon. In the premier government-run AIIMS, Delhi, the tuition fee is Rs.1,350 per year (A 2009 study Determination of the cost of training of MBBS student at AIIMS conducted by its department of hospital administration, estimates the cost of education provision in this top institute at Rs.31.31 lakh per annum per student). In Maharashtra, the government-run Seth Gordhandas Sunderdas Medical College in Mumbai, which has an enrolment of 2,000 undergraduate and postgrad students, charges tuition fees of Rs.20,000 per year.
Yet the great unchecked iniquity in medical education in contemporary India is that notwithstanding the corruption-driven conditionalities and curbs imposed upon the promotion of greenfield medical colleges by MCI and complicit government officials, state governments insist upon a reserved government quota in private medical colleges which successfully run the MCI-government obstacles race. Most state governments have enacted legislation to force private medical managements to surrender 40-50 percent capacity to government selected students at subsidised tuition fees. For instance in Karnataka, the state government has worked out a complicated three-tier tuition fees structure for private medical colleges under which 40 percent of students admitted through the government’s CET (Common Entrance Test) pay a mere Rs.35,000 per year; 40 percent of students admitted through the COMED-K (Consortium of (private) Medical, Engineering and Dental Colleges, Karnataka) test pay Rs.3.25 lakh per year; 15 percent NRI students pay Rs.10-12 lakh per year, with the remaining 5 percent seats auctioned by college managements. “It’s a structure designed to encourage corruption and extortion,” comments an embittered medical educationist.
 Government interference with the tuition fees fixation and admission processes of private professional (medical, engineering, business management) colleges continues despite the Supreme Court in its historic verdict in the T.M.A Pai Foundation (2002) case, permitting privately promoted professional colleges to prescribe their own admission procedures (subject to their being transparent and merit-based) and levy “reasonable” tuition fees. But a subsequent five-judge bench of the apex court in the Islamic Academy Case (2003), whittled down the court’s earlier verdict, allowing state govern-ments to establish admission and fees committees to supervise whether admis-sion procedures of private professional colleges are transparent and tuition fees levied reasonable. Since then, private professional (including medical) college managements have bought peace by voluntarily surrendering 40-50 percent of their seats to state governments at subsidised tuition fees.
Government interference with the tuition fees fixation and admission processes of private professional (medical, engineering, business management) colleges continues despite the Supreme Court in its historic verdict in the T.M.A Pai Foundation (2002) case, permitting privately promoted professional colleges to prescribe their own admission procedures (subject to their being transparent and merit-based) and levy “reasonable” tuition fees. But a subsequent five-judge bench of the apex court in the Islamic Academy Case (2003), whittled down the court’s earlier verdict, allowing state govern-ments to establish admission and fees committees to supervise whether admis-sion procedures of private professional colleges are transparent and tuition fees levied reasonable. Since then, private professional (including medical) college managements have bought peace by voluntarily surrendering 40-50 percent of their seats to state governments at subsidised tuition fees.
The fallout of 50 percent of students in private medical colleges paying tuition fees ranging from a mere Rs.20,000-35,000, and another 40 percent paying Rs.2-3 lakh per year (whereas actual cost of medical education as calculated by MCI is Rs.4 lakh per year), is the phenomenon of capitation fee. Unable to provide and upgrade infrastructure facilities, pay faculty salaries (which range between Rs.80,000-1 lakh per month) and maintain mandatory teaching hospitals, managements of private medical colleges make up the difference by levying capitation/dona-tion fees (repeatedly banned by the Supreme Court) upon students applying for admission under the 5 percent management quota. According to a news report in Deccan Chronicle (May 17), 19 private medical colleges in Andhra Pradesh are under the state govern-ment’s scanner for demanding capitation fees of Rs.1.5 crore for management quota seats.
“Private colleges need to invest in infrastructure including teac-hing hospitals. Besides, they have to pay huge salaries to faculty and doctors at the hospitals. Conse-quently, some private colleges resort to levying exorbitant tuition and capitation fees under the management quota. Whatever the reason, this needs to be checked and government interference is justified,” says Dr. T.P. Lahane, dean of the Maharashtra govern-ment-run Grant Medical College and JJ Group of Hospitals, Mumbai.
Dr. Lahane’s justification of government control of fees in private medical colleges is not a minority viewpoint. Middle class India’s addiction to subsidised higher education is well known, and heavily politicised student unions fiercely protest even small increases of ridiculously low tuition fees. But what they fail to understand is that the outcome of keeping fees at unrealistically low levels, covering as little as 10 percent of the operational cost in some institutions, is consistent decline in the quality of education dispensed by India’s medical colleges. Allocations for libraries, laboratories and information technology support for education and research are constantly shrinking, which has set India’s medical education system back by several decades and down-graded Indian medical degrees in several countries.
Belatedly as usual, the Union and state governments have become aware that there should be a quid pro quo for the rock-bottom tuition fees (medical education in government colleges in the US and China is priced at Rs.8 lakh and Rs.2.42 lakh per year) mandated for government and private colleges. Therefore, this summer the Union health ministry has announced a mandatory 12-month rural posting for all final year MBBS students, most from the elite and middle class who have cornered medical education for the past five decades. In a letter to MCI in May, the ministry has instructed its Board of Governors to make rural postings for doctors mandatory, and include it in the MBBS course curriculum. After MCI ratifies this proposal, the duration of the MBBS programme will increase from 5.5 to 6.5 years. Some state governments such as Maharashtra have already issued circulars stating that government medical college students who don’t comply with the rural service clause will have to pay up to Rs.10 lakh (MBBS), Rs.50 lakh (postgraduate) and Rs.2 crore (super-speciality students) respectively.
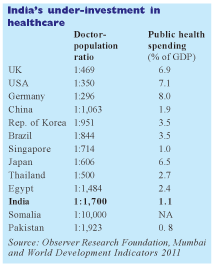
The rationale behind a year’s service in the country’s under-served rural outbacks is that with government spending on healthcare a mere 1.1 percent of GDP (cf. 7 percent in the US and 6.5-8 percent in the UK and other European nations), public health facilities and services in rural India are abysmal. Decently equipped hospitals and nursing homes are non-existent in the hinterland, with the over-whelming majority compelled to make do with a mere 23,391 government primary health centres (PHCs), of which only 38 percent are staffed by qualified medical personnel.
 Already some academics are questioning the rationale of this payback proposal. “Sending MBBS graduates to rural areas is not a solution. Students who paid lakhs of rupees to acquire seats in private medical colleges will never serve in villages. If the government wants to address the problem of shortage of doctors in rural and semi-urban areas, it must first establish reasonably well-equipped public hospitals and health centres, and improve rural infrastructure. Better connectivity with cities, electricity, education facilities, law and order are a pre-conditon of sending doctors and their families to rural areas. A better idea is to promote new medical colleges with attached teaching hospitals in rural districts with preference given to local students for admission,” says Dr. Arun Jamkar, vice chancellor of the Maharashtra University of Health Sciences, Nashik.
Already some academics are questioning the rationale of this payback proposal. “Sending MBBS graduates to rural areas is not a solution. Students who paid lakhs of rupees to acquire seats in private medical colleges will never serve in villages. If the government wants to address the problem of shortage of doctors in rural and semi-urban areas, it must first establish reasonably well-equipped public hospitals and health centres, and improve rural infrastructure. Better connectivity with cities, electricity, education facilities, law and order are a pre-conditon of sending doctors and their families to rural areas. A better idea is to promote new medical colleges with attached teaching hospitals in rural districts with preference given to local students for admission,” says Dr. Arun Jamkar, vice chancellor of the Maharashtra University of Health Sciences, Nashik.
Another Union health ministry initiative which has greater chance of success involves the introduction of a three-year bachelor of rural healthcare (BRH) study programme, which will create a separate cadre of public health professionals to serve in rural India. The BRH programme, which is also pending MCI approval, has already been introduced by some states including Assam and Chhattisgarh. “Doctors are opposing this new programme. I have no hesitation in saying that they have a vested interest to increase their practice. The curriculum is ready. States are free to implement the BRH programme as Assam is already doing, but we want the MCI’s help to prescribe uniform standards for this programme across India. We hope the MCI will move fast,” says Ghulam Nabi Azad, Union health and family welfare minister.
According to Azad, reforms in medical education is a top priority, with the ministry already having tabled the National Commission for Human Resources for Health Bill (NCHRH), 2011, in Parliament in December last year. The Bill, currently before a Parliamentary Standing Committee, proposes to subsume the MCI, Dental Council of India and Pharmacy Council. It provides for trifurcation of regulatory functions between three separate bodies viz, National Board for Health Education, National Evaluation and Assessment Committee and National Councils with a mandate to prescribe minimum standards for health education, develop and maintain accreditation systems for health education institutes, and inter alia monitor ethical standards among medical professionals. “NCHRH is progressive legislation. By dividing accreditation and regulatory powers between various constituent bodies, the Bill will reduce the corruption possible under an all-powerful single authority,” says Dr. K.K. Aggarwal, dean, Maulana Azad Medical College, Delhi (estb.1958).
However, NCHRH Bill, 2011 is being fiercely opposed by the medical fraternity with the Indian Medical Association (IMA), which boasts a membership of 178,000 allopathic doctors countrywide, staging a “medical bandh” on June 25. “The proposed National Commission for Human Resources and Health will not have any elected members and state representatives to voice their needs and demands. There is no provision also for representation from professional organ-isations such as IMA in the commission, board or councils, shunning the voice of healthcare providers. The IMA totally rejects the proposed NCHRH Bill,” says Dr. G.K. Ramachandrappa, president of IMA.
 The Bill is also being criticised for failing to integrate and mainstream the indigenous AYUSH (ayurveda, yoga, unani, siddha and homeopathy) systems. Comments Radha Viswanathan, co-author of Reforms in Medical Education — To promote Accessible and Affordable Healthcare for All (2012), published by Observer Research Foundation, a Mumbai-based think tank: “The Bill lacks any provision to mainstream the AYUSH and Indian systems of medicine which contribute to keeping healthcare costs affordable and are, in fact, healing systems of choice for a large section of the population. NCHRH should coordinate with the National Skills Development Corporation to train human resources other than doctors as per the require-ments of the healthcare industry. Moreover the Bill is silent on the subject of academic autonomy of institutions of excellence. Clearly, the Bill has been drafted in a hurry and needs thorough debate before it becomes law.”
The Bill is also being criticised for failing to integrate and mainstream the indigenous AYUSH (ayurveda, yoga, unani, siddha and homeopathy) systems. Comments Radha Viswanathan, co-author of Reforms in Medical Education — To promote Accessible and Affordable Healthcare for All (2012), published by Observer Research Foundation, a Mumbai-based think tank: “The Bill lacks any provision to mainstream the AYUSH and Indian systems of medicine which contribute to keeping healthcare costs affordable and are, in fact, healing systems of choice for a large section of the population. NCHRH should coordinate with the National Skills Development Corporation to train human resources other than doctors as per the require-ments of the healthcare industry. Moreover the Bill is silent on the subject of academic autonomy of institutions of excellence. Clearly, the Bill has been drafted in a hurry and needs thorough debate before it becomes law.”
Meanwhile MCI has prepared an ambitious ‘Vision 2015’ document titled Implementation of Reforms in Under-graduate and Postgraduate Medical Education. The document makes important curriculum reform recommen-dations, including a proposal to provide early clinical exposure to students, reduce the duration of the MBBS degree programme from four-and-a-half to four years by making subjects such as forensic medicine, ophthalmology and ENT optional; introduction of electives such as bio-informatics, tissue engin-eering/processing, computer applic-ations, immunology, to permit flexible learning options in the curriculum; adoption of contemporary education technologies such as skills laboratories, e-learning solutions, simulation, and establishing regional learning facilitation centres to enhance continuous faculty development programmes etc.
.gif) “The Central government and the newly constituted MCI are heading in the right direction. But the pace of reforms is too slow. It may take another 100 years before we see substantial changes in our medical education system. What we need are bold and decisive reforms in the country’s regulation and accreditation processes with liberalised norms and controls. Medical institutions which have established reputations should be given full autonomy to initiate curriculum reform, charge market-driven tuition fees and full freedom to administer their institutions,” says Dr. Ramdas Pai, chancellor of Manipal University which runs the premier Kasturba Medical College (KMC, estb.1953). Karnataka’s first private medical college, KMC has an enrolment of 500 students who are admitted through a transparent admi-ssion process and pay tuition fees of Rs.5 lakh per year. The college volun-tarily provides 28 seats for state govern-ment students at government fee norms.
“The Central government and the newly constituted MCI are heading in the right direction. But the pace of reforms is too slow. It may take another 100 years before we see substantial changes in our medical education system. What we need are bold and decisive reforms in the country’s regulation and accreditation processes with liberalised norms and controls. Medical institutions which have established reputations should be given full autonomy to initiate curriculum reform, charge market-driven tuition fees and full freedom to administer their institutions,” says Dr. Ramdas Pai, chancellor of Manipal University which runs the premier Kasturba Medical College (KMC, estb.1953). Karnataka’s first private medical college, KMC has an enrolment of 500 students who are admitted through a transparent admi-ssion process and pay tuition fees of Rs.5 lakh per year. The college volun-tarily provides 28 seats for state govern-ment students at government fee norms.
Radha Viswanathan (quoted earlier) of the Observer Research Foundation also believes that India needs a completely new regulatory system for medical education. “History has shown that excessive regulation has increased malpractices instead of curbing them. It is time therefore for a paradigm change — to make the rules more liberal and focus on penalising wrongdoers rather than constraining everyone uniformly. For too long, regulation in India, particularly in the education sector, has been about prescriptive policies. In the quest to maintain minimum standards, we have over-specified norms and only succeeded in producing a common denominator that is far beneath world standards, while crushing grassroots innovation. It is now time to make a break from this approach and initiate a quest for excellence, to create an environment in which leading educa-tional institutions are at the forefront of this quest, by becoming autonomous and working towards making themselves nationally and internationally compet-itive,” says Viswanathan.
Indeed a complete overhaul of the medical education licensing and regulatory system rather than band-aid solutions are required to restore public faith in the country’s 355 medical colleges and MCI, reeling under a rash of corruption scandals. With one of the worst doctor-population ratios world-wide, India urgently needs a regulatory environment which encour-ages private sector initiatives and capacity expansion to meet the growing shortage of human resources in the health sector. Moreover, the Union and state governments must immediately triple GDP spending on health from the current 1.1 to 3.3 percent, strengthen the country’s 23,391 PHCs and community health centres, and build adequate healthcare infrastructure in rural India. The allocation of Rs.404,000 crore in the 12th Plan Period (2012-17) — 2.5 percent of GDP — is a good augury but still way short of the 6-7 percent spent by progressive Western nations.
The silver lining of the unprecedented quality crisis in medical education and deplorable state of public healthcare in rural India, is the opportunity it offers for root-and-branch reform. The onus is on all actors — the Central and state governments, MCI, medical college managements and faculty and student communities — to work purposively to ensure it’s not missed again.
With Praveer Sinha (Mumbai) & Baishali Mukherjee (Kolkata)